Learninsta presents the core concepts of Microbiology with high-quality research papers and topical review articles.
Mycobacterium Tuberculosis (Tubercle Bacillus)
The genus Mycobacterium is distinguished by its thick, complex, lipidrich waxy cell walls. This high lipid content (Mycolic acids) imparts the characteristic of acid fastness or resistance to decolorization by a strong acid after staining with carbol fuchsin. Many of the Mycobacterial species are saprophytes but several species are highly significant human pathogens.
Mycobacterium tuberculosis is the causative agent of tuberculosis (TB) It is a killer disease and ranks as one of the most serious infection diseases of the developing countries. TB is primarily a disease of the lungs but may spread to other sites of the body.
The name Mycobacterium tuberculosis is derived form,
- Mycobacterium (Greek) – Fungus like bacterium
- Tuberculosis (Latin) – Swelling or Knob
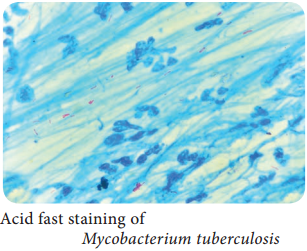
Morphology
They are acid fast bacilli, slightly curved rods, it may occur singly or in small clumps. They are non-motile, non-sporing, and non-capsulated.
Cultural Characteristics
They are obligate aerobe, optimum temperature is 37°C and optimum pH is 6.4-7.0. The pathogen grows on an enriched culture media – Lowenstein Jensen medium.
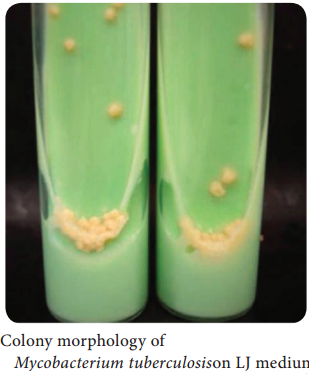
The colonies appear in about 2-3 weeks. The colonies are dry, rough, raised, irregular colonies with a wrinkled surface. Initially creamy white and becoming yellowish later (Figure 7.19).
Pathogenesis
Human tuberculosis is divisible into two form, they are Primary TB and Secondary TB. The pathogenesis of Primary Tuberculosis is described in flowchart 7.8.
Source of infection – Airborne droplets
Route of entry – Respiratory tract
Incubation period – 3 – 6 weeks.

Secondary TB – (Post primary TB)
It is caused by reactivation of the primary lesion or by exogenous reinfection. Granulomas of secondary TB most often occur in the apex of the lungs. The necrotic element of the reaction causes tissue destruction and the formation of large area of caseation termed tuberculomas.
The presence of caseous necrosis and cavities are two important clinical manifestations of secondary TB. The cavities may rupture into blood vessels, spreading the bacilli throughout the body and break into airways, releasing the pathogen in aerosols and sputum – called as open tuberculosis (Figure 7.20).
Clinical Symptoms
It includes, cough that lasts for more than 2-3 weeks, weight loss, fever, night sweat and loss of appetite.
Laboratory Diagnosis
Specimen:
In case of pulmonary tuberculosis the most usual specimen is sputum.
Direct Microscopy:
Smear is made from the sputum specimen and stained by Ziehl – Neelson technique. It is examined under oil immersion objective lens. The acid fast bacilli appear as bright red bacilli against a blue background.
Culture:
The specimen is inoculated onto LJ – medium and incubated at 37°C for 2 weeks the tubercle bacilli usually grow in 2-8 weeks. The bacterial growth is confirmed by Ziehl – Neelsonstaining.
1. Tuberculin Skin test
Mantoux test:
This method has been used routinely. In this test 0.1 ml of PPD (Purified protein derivative) containing 5 TU (Tuberculin unit) is injected intradermally on the flexor aspect of forearm (Figure 7.21) The site is examined after 48-72 hours and induration are measured (diameter in mm).
Positive test:
Indurations of diameter d10 mm or more is considered positive.
Negative test:
Indurations of 5 mm or less is negative.
2. Gene Xpert MTB
It is an automated diagnosis test it detects DNA sequences specific for M. tuberculosis and rifampicin resistance by PCR. Results can be obtained within 2 hours.
Treatment
The antitubercular drugs include two types of agents which are;
Bactericidal agents – Rifampicin (R), Isoniazid (H), Pyrazinamide (z), Streptomycin.
Bacteriostatic agents – Ethambutol (E).
The regimen for treating TB consists of an intensive phase of 2 months of isoniazid, rifampin, pyrazinamide and ethambutol, followed by a continuation phase of 4 months of isonizid and Rifampin.
Prophylaxis and Control Measures
The BCG (Bacille – Calmette – Guerin) administered by intradermal injection of the live attenuated vaccine. The immunity may last for about 10 years. The prevention of TB can be done by the following general measures such as
- Adequate nutrition.
- Practicing good hygiene (washing hands)
- Health education.
- Cover the mouth with a tissue when you cough or sneeze.